
Starting in the mid-1950s, with the research of Ancel Keys, saturated fat became accepted as one of the primary causes of cardiovascular disease (CVD). The first low fat dietary guidelines were implemented in the US in the mid-1970s, with highly questionable health effects over the last 30 years. But, research has never been able to find evidence to fully support the saturated fat theory. Luckily, due to emerging research there has been a shift in recent years linking other dietary factors to CVD risk. If you have read this blog for any period of time, you probably know where I stand on this topic already.
The interest in this area of nutrition research continues because cardiovascular disease remains the number one cause of death in the United States. Finding a cause of this disease can hopefully help us find a cure. As a dietitian it is important for me to stay on top of the latest research on this topic and a recent study intrigued me because of a slightly different approach in how they determined exactly what people eat. The correlational study published in March 2018 in Nutrients sought to look at the connection between diet and CVD from a global perspective using food availability data and the results were quite interesting.
Before diving into the results of the study itself, let’s talk a little bit about correlational studies in general. A correlation study simply identifies a possible connection between two variables and should not be interpreted as having found a direct cause.
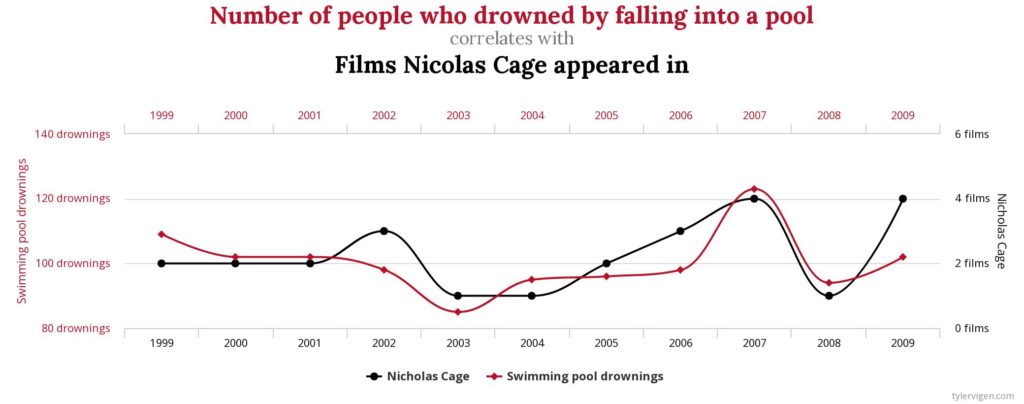
One of my favorite graphics, from a website dedicated to discovering interesting correlations, is the connection between divorce rate in the state of Maine and margarine consumption. As you can see by this graph, as margarine consumption decreases so do divorce rates.
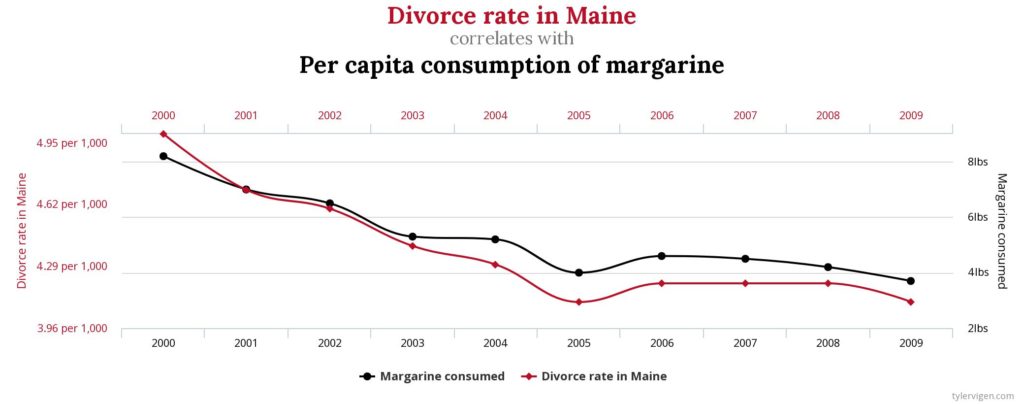
Clearly, these two variables are not actually connected at all. There must be other variables at play here, but you can see that based on the statistical analysis a correlation or connection seems to exist between the two. So, correlations, albeit interesting, are not always accurate and further investigation is needed with correlational data to determine if there truly is any causation between two variables.
In looking at the data from the March 2018 study on CVD (and many other similar nutrition studies) take into account that depending on how the study is designed, researchers are only able to discover potential connections between variables, not actual direct connections. In light of this information about correlational studies, let’s dive in to the study itself and how it is slightly different from many other nutrition studies.
“Global Correlates of Cardiovascular Risk: A Comparison of 158 Countries” utilized data from the Food and Agriculture Organization Corporate Statistical Database (FAOCSD) to analyze food availability and predict food consumption in order to correlate it with risk of CVD. Most studies to date on diet and CVD risk use self-reported diet records or food frequency questionnaires both of which are notoriously inaccurate. This particular study included an analysis of over 60 foods and their connection with several variables linked to heart disease including high blood pressure, body mass index, cholesterol levels, life expectancy, health expenditure, elevated blood glucose, and CVD mortality rates.
With this slightly different methodology of evaluating food consumption here are some of the primary results:
– Intake of high glycemic carbohydrates, particularly wheat, were most positively correlated with CVD incidence and high blood pressure across all countries, even when controlling for other variables such as health care expenditure.
– Alcohol intake and sunflower oil were also positively correlated with CVD risk, although less than carbohydrates.
– Total fat and animal protein intake were found to have a strong negative correlation with CVD death risk, particularly in Europe. But, when controlled for health expenditure, this correlation was no longer significant.
– High blood pressure was most correlated with intake of cereals and starchy roots, particularly in women. Interesting to note, this was not found in Asian countries where the primary cereal/grain is rice, but in countries where they consume mostly wheat and maize.
– For women, blood pressure was negatively correlated with high cholesterol, animal protein intake, and life expectancy.
– In Europe, total fat and animal protein was negatively correlated with high blood pressure.
– The strongest positive connection between elevated cholesterol and diet were found with animal fat and animal protein, followed by % of calories from plant foods.
– Elevated blood glucose was most correlated with CVD death, obesity, and also with the consumption of grains, especially wheat.
– High blood sugar is negatively correlated with alcohol and pork intake, which was surprising. But, the data is slightly skewed showing a much stronger negative correlation because both of these foods are prohibited in Muslim countries, that also tend to eat a large amount of cereals and have high obesity rates.
– In every country other than Europe, carbohydrate intake is weakly associated with high blood glucose. But, the reason may be that in many developing countries, even though the carbohydrate intake is proportionally high in the diet, malnutrition and poverty are prevalent, making carbohydrate intake actually moderate in terms of quantity and obesity is very low, impacting blood glucose.
– Smoking is the most strongly correlated variable with CVD mortality, especially for men. Interestingly, the correlation between CVD death and smoking for women is negative, but there are confounding variables in that usually only women in wealthy countries smoke where there are other protective factors at play.
– For men, alcohol and potato intake are the most strongly associated dietary factors with CVD risk. This may be a bit skewed by including data from the USSR where alcohol is made from potatoes and alcoholism is a major problem in men.
– Interestingly, in the countries that spend the most money on healthcare, very few strong correlations are found between diet and CVD mortality. Researchers believe the data was skewed by certain countries such as Japan and South Korea consume a lot of carbohydrates, but have lower risk of CVD mortality.
Lastly, there are a few limitations of this study that should be discussed. First, many of the countries analyzed did not have sufficient data on CVD mortality or consumption of certain types of foods to really do a thorough analysis of the correlation between these two factors. Also, several countries had a very low intake of some of the foods as well as high rates of malnutrition making it difficult to determine if there was any effect of diet on CVD risk.
According to the authors of this study, food availability data has not previously been used to determine actual food consumption and its connection to disease risk. The results of this study are interesting and point to a connection between carbohydrate intake and CVD risk, more so than saturated fat intake. But, with this being a correlational study further research is needed to determine if there is a true connection between a high glycemic diet and risk of CVD death. Regardless, this is an interesting study that can be used to help guide researchers to truly determine the diet-related causes of CVD.








3 thoughts on “New Global Study Links Carbohydrates (Not Fat) Heart Disease”
“Researchers believe the data was skewed by certain countries such as Japan and South Korea [which] consume a lot of carbohydrates, but have lower risk of CVD mortality.”
In point of fact, I know from friends and acquaintances who have lived in those countries, that in China, South Korea and Okinawa, the amount of carbohydrate (i.e. rice) sold does not correspond to the amount consumed.
In those countries, the traditional way of dining involves individual bowls of rice, and a communal meat and vegetable dish. Diners serve themselves from the communal dish onto the top of their individual rice bowl, then eat down to the rice, consuming only as much of the latter as has absorbed the sauce. They then serve themselves again, from the first or another communal dish, and repeat the process.
At the end of the meal, it is rare for more than half of the rice to have been consumed. The balance, in rural areas at least, goes to the pigs!
This may help resolve the apparent contradiction in the statistics.
Yes! Food availability and consumption are different numbers! I’ll go back and see if the numbers are based on estimated consumption or simply availability.
First of all, I would like to thank Diana that she sacrificed a lot of time to the reading of this long text and understood all its main points. I was afraid that many people won’t be able to do it.
And as for rice: Yes, there is a problem between food availability and true food consumption – the latter being relatively lower in wealthy countries where food abundance leads to greater food waste. Still, these data reflect true food consumption with much higher accuracy than any self-reported data based on food questionnaires. And second, the disproportionately weaker association between rice and CVD applies to all rice-consuming regions of South and East Asia, so the possibility that Japanese and Koreans do not eat all rice in their dishes is not a plausible explanation.